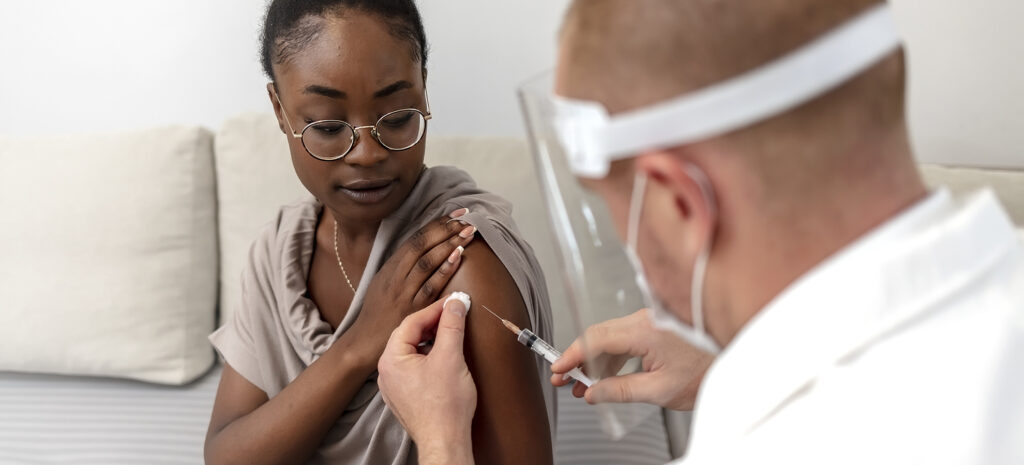
The life science sector relies on the clinical trial process to ensure that drugs, compounds, and medical devices are safe and effective. To do so, clinical trials must be representative of the wider population and encompass as broad a range of people as possible. But there’s a problem. According to the FDA, 75% of US clinical trial participants are white. They’re also predominantly male, with the British Medical Journal reporting that just ≈22% of phase 1 patients are women.
“Any clinical trial that assesses such a narrow subset of people will fail to produce a full picture of a drug’s efficacy or safety.”
In this article, we’ll explore why there’s a lack of diversity and inclusion in clinical trials, and examine how technology can help redress the balance.
Biases and barriers to inclusion
The reasons behind the lack of clinical trial diversity are varied and complex. The FDA, for example, banned certain women of childbearing age from participating in clinical trials in the wake of the Thalidomide scandal of the 1950s and ’60s. While these guidelines were rescinded in 1993, women remain underrepresented in clinical trials to this day.
Meanwhile, certain chronic conditions are prevalent among underrepresented populations. For example, 20% of US myeloma cases are found among African-American people, but only 6% of clinical trial participants are black. Unconscious bias plays a part in the lack of clinical trial diversity, but there are numerous barriers to participation that must be overcome to ensure greater representation in clinical trials.
Related content: Confronting the Life Science Diversity Problem
These barriers include physical distance, with the average patient traveling 25.8 miles for clinical trial visits, according to The Oncologist. Many remote or rural communities are also often home to a higher proportion of low-income families, making financial issues another barrier to inclusion. Among minority ethnic groups, there are sometimes language barriers to contend with, as well as historical mistrust of clinicians.
“53% percent of non-Hispanic white participants said that they trusted their health professionals ‘a lot,’ compared with 37% for non-Hispanic black participants and 36% for Hispanic participants.”
Medical News Today
These barriers to participation mean that women, people from minority ethnic backgrounds, and members of lower socio-economic groups remain underrepresented in clinical trials – with the result that we can’t always be certain how new drugs, devices, and compounds will interact with the broader population.
“As such, many underrepresented groups can expect worse prognoses – with black people suffering higher death rates than white people for 12 of the 15 most common causes of death in the United States, per the National Press Foundation.”
Addressing trial diversity through technology
Improving clinical trial diversity and inclusion means removing the barriers to participation that prevent underrepresented groups from taking part. Life science companies must be willing to enact these changes, but emerging digital technologies are already helping to make clinical trials more diverse and representative.
Understanding disease communities with network analytics
“Network analytics can be a valuable tool to learn about how governance structures, communication channels, and trust between member organizations make it easier to work towards a shared goal, like improved community health or narrowing gaps in racial health inequities.”
Health Leads
Network analytics allows life science companies to understand the relationships within disease communities: how HCPs and experts interact, how they’re connected with patients, and where all these different individuals are based. This knowledge allows clinical teams to make more informed decisions on site selection, based on the real-world locations of target patient populations. According to McKinsey, more than 70% of patients live over two hours from trial sites, so providing more convenient site access removes a significant barrier to participation.
Identifying trial participants with artificial intelligence
“AI capabilities, including natural language processing and association rule mining, help extract data to find patients suitable for clinical studies, and can help identify those most likely to complete a trial.”
Icon
Artificial intelligence (AI) has already proven successful in clinical trial recruitment, with Forbes reporting that “an AI-enhanced trial at Cedars-Sinai identified 16 candidates in one hour, while a human-based approach found two people in six months.” As well as patient identification, AI applications such as natural language processing and sentiment analysis can also be used to identify trends and sentiments from patient interactions, helping clinical teams better understand the needs of trial participants.
Hearing the voice of the patient with social listening
“The average clinical trial dropout rate is 30%”
Clinical Leader
Effective recruitment is just one aspect of clinical trial diversity and inclusion. Trial retention is another.By analyzing social media and other online data sources, social listening can be used to provide a window into the patient experience. Highlighting what patients and HCPs are talking about allows clinical teams to assess which barriers to participation, if any, are affecting their target populations, and enables them to address concerns that could lead to dropouts further down the line.
Enabling decentralized trials with asynchronous engagement
Asynchronous virtual engagement is helping to democratize the clinical trial process, connecting clinical teams with underrepresented communities without the need for expensive, time-consuming travel to and from trial sites. By enabling decentralized clinical trials – which require fewer or even no in-person clinical visits – asynchronous virtual engagement removes some of the most significant barriers to trial participation. Decentralized clinical trials require patients to carry out tests and procedures themselves at home, so frequent contact between participants and clinical teams is essential. Asynchronous virtual engagement allows this to happen at a time and place that works for them.
Life science organizations have a duty to address diversity and inclusion throughout the drug development process, in the boardroom and beyond. Discover the four technologies helping to address issues of diversity in life science in our ebook: Confronting the Life Science Diversity Problem.